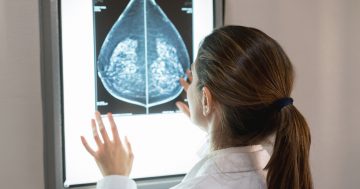
Doctors say it’s time the ACT had a specialist women’s cancer treatment centre. Photo: File.
Doctors have hit out at the ACT Government’s suggestion that Canberra is too small to sustain a specialist women’s cancer treatment centre.
Currently, women who require surgery for gynaecological oncology surgery and clinics have to travel to Sydney for critical treatment and recovery.
They have been supported by Dr Greg Robertson from the Royal Women’s Hospital in Sydney who has been travelling to Canberra for more than 20 years to provide some of these specialist services.
But the fortnightly clinic has too many patients who need access so most patients still travel for operations and post-operative care.
Dr Robertson said his retirement at the end of the year will mean Canberra is left without these services.
“Patients with gynaecological cancer will have to find another opportunity of accessing care and support,” he said.
It’s now been three years since a group of doctors started lobbying the federal government to improve cancer services for Canberra women, bringing the issue to the attention of the ACT Government earlier this year.
In this time, they claim both governments have failed to make any commitment to establish comprehensive treatment for women in the region despite the fact there are no conditions affecting only men that cannot be cared for in the ACT.
Specifically, Dr Robertson wants to see the ACT establish a permanent and local multi-disciplinary team for gynaecological cancers – which he said is the same level of care already provided for other cancers, such as prostate, breast and colon.
One of the main arguments against establishing that team and centre – as put forward by the ACT Government – is that Canberra is simply too small.
Dr Robertson, however, “respectfully disagrees”.
“The ACT doesn’t sit alone here. There are also all of the surrounding areas like Goulburn, Yass and the South Coast, which already use Canberra to access all of their specialist healthcare services,” he explained.
“When you add our population to all of that region, it would certainly justify such a service.”
When Dr Robertson does retire at the end of this year, another doctor, Leon Foster, is ready to step in and run a clinic. Dr Foster will complete the additional training required later this year.
The doctors warn that another opportunity like this may not come up for another 10 to 20 years given how highly specialised the training is.
In the entire country, there are only 60 doctors qualified in the field of gynaecological oncology surgery.
“It’s not a huge investment either, compared to what they spend on other things,” Dr Robertson said.
Gynaecological cancers are also not that rare. Dr Robertson treats around 100 new patients every year.
The statistics say one in 20 women will develop gynaecological cancer in their lifetime, and ovarian cancer is the sixth most common cause of cancer deaths in females.
Of more concern for Dr Robertson is that he sees many patients who don’t present until they are in an emergency situation.
“Their care has been delayed because they haven’t had access to a gynaecological oncological service which would otherwise decrease the amount of time they need to spend in hospital,” he explained.

Health Minister Rachel Stephen-Smith said Canberra Health Services is working alongside specialists to expand gynaecological cancer services. Photo: Thomas Lucraft.
The Territory’s Health Minister Rachel Stephen-Smith said Canberra Health Services (CHS) is working on expanding care for gynaecological cancer services in the ACT alongside specialists like Dr Robertson and Dr Foster.
“We recognise that it creates stress and strain when people need to travel for care,” she noted.
“But there are a number of specialist services that we are just not able to deliver in the ACT because we don’t have the population to support them.
“It’s important that people delivering these services get enough throughput so they can sustain their skill level in these services.”
The Health Minister acknowledged Canberra’s population is growing and said it was being factored into future plans, but that right now, even when considering the surrounding region’s population, Canberra was still much smaller than even Western Sydney.
She rejected claims it was a question of funding, instead saying it was about being able to recruit and retain the right specialists and support staff to deliver the service safely.