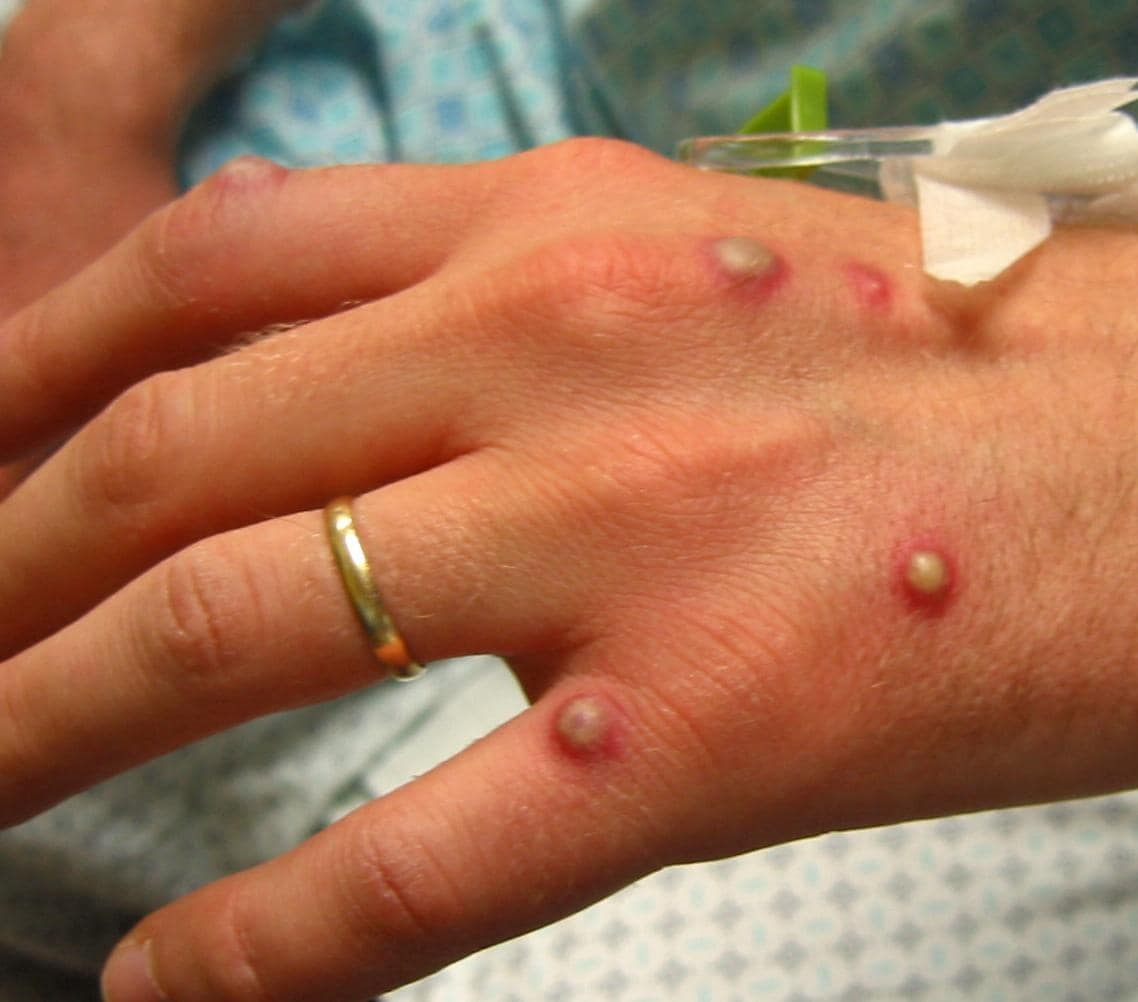
Monkeypox rash usually develops following fever, chills and swollen lymph nodes, and spreads across the body. Photo: Medscape.
“Let’s have some perspective: these viruses have been around a long time, that doesn’t necessarily mean they cause major epidemics.”
That’s the advice from ANU epidemiologist Professor Peter Collignon when asked about monkeypox.
In recent weeks the virus has been reported in numerous countries where it’s not usually found, including Europe, the United Kingdom, United States and Canada.
It’s also been detected in Australia, with three cases now confirmed in NSW and another in Victoria.
But that doesn’t mean there’s cause for alarm.
“We’ve known this has been in Africa since at least the 1970s, but it’s probably been present there for years and years even before then,” Prof Collignon said.
“There are cases all the time. Someone said to me the other day it’s only when it affects rich countries that people get excited about it.”
While Prof Collignon said the reason for its spread from Africa was unknown at this stage, it’s not a disease that’s easily shared.
“So far it’s been identified in very close contacts,” he said.
“It can also be spread from rodents. There was an outbreak of about 37 cases in the US in 2003 and that was from imported prairie dogs.
“This spreads much, much less than COVID.”
Prof Collignon could understand why we may be a bit jumpier about viruses we’re not familiar with due to COVID-19 but gave his reassurance that while nobody is at “zero risk”, a person’s chance of catching monkeypox was “very, very low”.
“So far there have been about 300 cases reported worldwide,” he said. “If this could readily spread we would already see cases in their thousands.
“It’s actually not easily diagnosed … because of COVID we’re out looking for diseases, we have more molecular technologies such as PCR testing more readily available as well to diagnose.
“This could have easily spread without us even knowing about it, unless you do a genomic analysis you wouldn’t know what it is.”
He also noted less than one per cent of people die from monkeypox and most recovered without any medical intervention at all.
“So you can be alert but we shouldn’t panic about it,” Prof Collignon said.
“It carries much, much less risk than COVID or any other respiratory disease.”
ACT Chief Health Officer Dr Kerryn Coleman also stressed monkeypox was a “rare viral infection” that usually required direct skin-to-skin or prolonged face-to-face contact.
“Illness associated with the monkeypox virus is usually mild, although complications can occur,” she said.
Symptoms initially include a fever, chills, muscle aches, backache and swollen lymph nodes.
“Following these symptoms a rash usually develops that spreads to other parts of the body,” Dr Coleman said.
“The rash changes and goes through stages, like chickenpox, before finally becoming a scab.”
Dr Coleman said if you did experience such symptoms, you should stay at home and call your GP to organise a telehealth appointment.
The Canberra Sexual Health Clinic was another option, which can be reached on 5124 2184.
Dr Coleman said if you needed to attend an appointment in person to be diagnosed, you should wear a mask and cover any lesions.
“It is extremely rare to have monkeypox if someone has not travelled to endemic countries or come in physical contact with a person who has monkeypox disease.”
No cases have been reported in the ACT at this time, however local GPs and hospitals have been given advice on referral and diagnosis.
According to the World Health Organisation’s (WHO) latest report (26 May), rare cases of monkeypox in non-endemic countries were usually linked to travel to endemic countries. However, it stated most of the current cases didn’t have a history of travel to such countries.
“Therefore, the current outbreaks are unusual and different from previous travel-related outbreaks,” the report stated.
As of 26 May, 257 laboratory confirmed cases and about 120 suspected cases had been reported to WHO.
The majority of reported cases presented through primary care or sexual health services.













