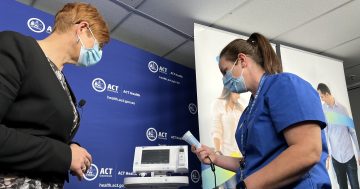
Belinda Vandermeer and Laura Curran are two of around 1600 super users who are being trained ahead of their colleagues in the Digital Health Record which will go live in two months. Photo: Lottie Twyford.
In less than two months, a Digital Health Record (DHR) will go live at the hospital.
The $150 million project will collate paper and digital patient records which are currently held across 40 different systems.
But before it can go live, a whopping 14,000-plus healthcare staff across the Territory’s public system will need to be trained to use it.
The first swathe of that – training around 1600 ‘super users’ – is already underway.
Canberra Health Services NDIS nurse project officer Belinda Vandermeer and Calvary Public Hospital senior speech pathologist Laura Curran are among that cohort.
The super-users won’t receive any more training than their colleagues. Instead, they will just be trained slightly ahead of everyone else so they can assist once the system is up and running.
Ms Vandermeer said the four sessions she had undertaken so far had been very useful.
“Each of the classes had built on the previous one. They are all relatively different parts of the system – and not everyone will need to learn all of them – but each time, I can see how everything connects,” she said.
“The progression for me when I’m looking after a patient or looking for information is all really easy.”
Staff will be trained in the use of the DHR during work hours and extra staff are being brought in from agencies to backfill shifts.
Ms Curran, who currently works on a paper-based system, said going digital would be a “huge change”.
“That’s not just from a documentation point of view, it’s being able to see a patient’s information across all of the different health services in one go,” she said.
“You won’t need to log in to a different system or actually go look up a paper record in an archive somewhere – it’s going to make my job faster.”
This was seconded by Ms Vandermeer, who said she often has to have multiple screens and apps open at once. With the DHR, this will all be in the same place.
That time-saving measure means clinicians can spend more quality time with patients and see more patients in one day.
“We will be able to spend more clinical time with the patient because that basic information is [on the DHR] and we won’t need to rewrite it over and over again,” Ms Vandermeer said.
“I don’t know how many times people write the same thing.”

Minister for Health Rachel Stephen-Smith said the future of medical transcriptionists would be further discussed next February. Photo: Thomas Lucraft.
The government has confirmed no jobs will be lost due to the introduction of the new system, but that hasn’t allayed the fears of medical transcriptionists who worry their jobs will be entirely different once the system goes live and an automated transcription voice-to-text program is implemented.
Last week, Health Minister Rachel Stephen-Smith said clinicians would be able to use transcriptionists if they would rather that than the new software.
But she indicated those roles would be up for consideration early next year following a three-month implementation and trial period.
“In February, further conversations will be had about … the need for transcription services into the future,” Ms Stephen-Smith said.
“But Canberra Health Services is having very detailed conversations with all of the staff that are involved in the transcription team to ensure they understand what these processes are going to look like and to reassure them how important they are to the organisation and their services will continue to have a role.
“It may change a bit, but we don’t actually know what that is going to look like at this stage.”
The Digital Health Record will also have a client-facing element people can use to book appointments and receive correspondence. That additional functionality will be rolled out following the initial ‘go live’ date.