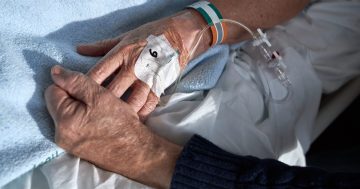
Human Rights Minister Tara Cheyne (second from left) said work would continue on the voluntary assisted dying legislation with stakeholders such as Go Gentle Australia CEO Dr Linda Swan, Katarina Pavkovic, Corinne Vale and Exit ACT chapter leader Dr David Swanton. Photo: Claire Fenwicke.
CONTENT WARNING: This article discusses suicide.
Katarina Pavkovic had to watch her father intentionally not eat food for five weeks when he decided he didn’t want to live anymore.
He had been suffering from Parkinson’s disease and had reached the point where he could no longer walk or talk, but he also wanted to die on his own terms.
“Towards the end, he could no longer face the intolerable suffering,” Katarina said.
“[He] would absolutely be smiling at the outcomes here today.”
That’s because now, just 11 months after Territory rights were restored, the ACT Government has introduced the Voluntary Assisted Dying Bill 2023.
Human Rights Minister Tara Cheyne introduced the proposed legislation to the Assembly on Tuesday (31 October). She said it was the greatest honour of her life.
“This bill is what we spent 25 years fighting for our Territory rights for,” she said.
“Voluntary assisted dying [VAD] is not an alternative to, nor does it detract from palliative care.
“It allows eligible individuals to make informed choices when they are at the final stages of their illness … it is not a choice between life or death, it is an additional choice.”
Extensive community and stakeholder consultation has taken place to formulate the proposed law, which allows access to VAD if a person is aged 18 years or older and:
- has a condition that is advanced, progressive and expected to cause death
- is intolerably suffering
- has lived in the ACT for 12 months, or be provided an exemption by demonstrating they have a substantial connection to the ACT
- is acting voluntarily
- has decision-making capacity throughout the process.
All of these eligibility requirements must be met, with the individual required to undergo a multi-step request and assessment process, with the assessment conducted by two independent and suitably qualified, trained and authorised health professionals.
One significant difference between the ACT’s scheme and other jurisdictions is that an expected timeframe to death does not need to be established.
Ms Cheyne said while it would have been simple to “copy and paste” the timeframe from other jurisdictions, removing this requirement was important.
“A timeframe to death is an arbitrary and unnecessary aspect of other state’s models,” she said.
“It’s very difficult in some circumstances and some illness for doctors to be able to accurately determine the timeframe to death for a person.
“[This will reduce] an individual’s intolerable suffering, as well as the stress and difficulty in having to request voluntary assisted dying very close to death.”
Another difference will be allowing experienced nurse practitioners to access the training to administer the VAD health service.
The bill does not mandate anyone take part in VAD but establishes minimum standards that must be followed by individuals and organisations, such as aged care homes and hospitals that conscientiously object to or cannot assist with voluntary assisted dying, not hinder access to VAD.
Katarina wishes her father could have been able to access the same option.
“It just would have eased suffering, not only for him but for everyone else around him,” she said.
“It would have given empowerment. It would have given choice, dignity and given us all the ability to say goodbye on our own terms.”
The government had been considering opening up the scheme to children aged 16 to 17 but decided not to pursue this option in the legislation presented.
A Select Committee on the bill has been established to examine the proposed law before it is debated. It must report by 29 February 2024.
It’s expected the VAD scheme will begin 18 months after the legislation passes to give enough time to set up this new health service with the necessary systems, safeguards and processes.
Some are concerned this time period will impact families who need to access the health service now.
Corinne Vale’s mother took her own life in April while she was receiving palliative care for motor neuron disease.
“She made the decision really quickly after her diagnosis that she wanted to be the one who decided when her suffering became intolerable and when it was time to call it quits,” she said.
“If she had known at the time of her diagnosis that voluntary assisted dying was available to her, it would have immeasurably improved the remaining months of her life.
“She could have focused on enjoying that time with those of us who loved her rather than researching ways to take her own life … because of the choice she made, I couldn’t be there when she died, I couldn’t hold her hand and tell her that I loved her.”
Corinne has been speaking with ministers on whether an interim option can be established so that people can access other VAD schemes across the border in the meantime.
“If someone you love tells you that they don’t want to ride their terminal illness all the way to the end … and the palliative options don’t meet their needs, it’s important they have the option to control the manner and timing of their passing,” Corinne said.
“For my mum, she wanted that choice.”
The scheme will be reviewed after it has been in operation for three years.
Further information on voluntary assisted dying in the ACT is available online.
If the issue of voluntary assisted dying raises issues for you or your family, you can contact Lifeline on 13 11 14 or Griefline on 1300 845 745.