Murrumbidgee Local Health District chief executive Jill Ludford. Photo: Supplied.
It takes a steady hand at the tiller to steer a vessel through a storm, and right now, in the southern reaches of NSW, the health of 250,000 people depend on it.
One person who has held unwavering eyes on the horizon is Jill Ludford, especially recently as the blustery tempest that is COVID-19 skulks on the border of NSW and Victoria
As chief executive of Murrumbidgee Local Health District (MLHD), Jill is used to critical situations. During the past 12 months she has stepped from dust storm to firestorm and then to the loitering storm of COVID-19.
For Jill, it’s all about keeping everyone safe. Not just the 3900 staff and thousands of patients under her watch, but every person in the vast health district that spans 125,243 square kilometres of southern NSW, stretching from the Snowy Mountains in the east to the plains of Hillston in the northwest, and all the way along the Victorian border.
“Considering the impact of the bushfires and now COVID-19, it has been a really challenging year,” she says. “I don’t think in seven months you’d ever imagine going through something like this on top of drought.”
The past summer’s bushfires threatened the lives and homes of MLHD patients and staff, forcing evacuations of towns and health facilities.
“The level of trauma our staff went through during that process has been enormous,” says Jill.
“Often these things go away from the public’s eyes, but it still remains up to us as an organisation to look after the wellbeing of our staff and also the long tail of these events in the community.”

MLHD chief executive Jill Ludford has faced the press alongside NSW Police Riverina District Commander Bob Noble for much of the past seven months since the outbreak of COVID-19 in Australia. Photo: MLHD.
By the time MLHD staff came up for air in late January 2020, the first COVID-19 case was diagnosed in Australia.
Almost every day since, Jill Ludford and her staff, alongside NSW Police, have resolutely fronted the media, opening a river of information which has helped contain the spread of the virus.
Innovation has also played its part, with 300 wearable devices flown in from Switzerland which allows local health professionals to remotely measure a patient’s vital signs, including heart rate, blood oxygen and skin temperature. This permitted home isolation and preserved the capability for hospital care.
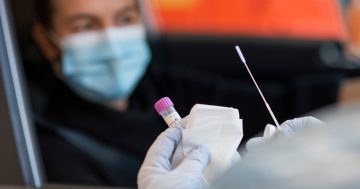
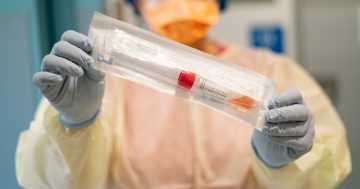
Proving its agility and flexibility in addressing the tyranny of distance, MLHD was first to trial mobile testing, zeroing in on COVID-19 hotspots while supporting isolated communities with limited capacity.
As commercial flights to Wagga Wagga and Griffith ground to a halt – preventing the daily inflow of medical specialists – Jill was able to leverage a relationship with the Royal Flying Doctor Service (RFDS).
Ongoing simulation training in each of MLHD’s 45 health care facilities remains a daily, if not weekly, undertaking. MLHD has tripled intensive care capabilities and has trained extra staff in preparation for new COVID-19 outbreaks.
Working beside Jill are staff who are unceasingly solution driven.
“They were the people who said we could do this and do it safely,” she says. “This is a medically led response to a disease, and our medical staff – our nurses, doctors and clinicians – know the best way.
“The challenge for us, when things go quiet again, is keeping those people razor sharp and ready to respond.”
Jill says acting decisively, openly and transparently has provided a level of comfort repaid in volumes by a community that has been exemplary in its compliance with public health orders.
“People have just said, ‘We’ve got to do this; it’s not easy, but we’ll do it,’” she says.
“We’re lucky because we can involve people more than you can in big cities. I’ve worked in Sydney and Canberra and you are quite separate from the community you are serving in cities.”
In regional areas, says Jill, people have a sense of ownership for their health facility and they admire the people who work there, which cushions many people during a crisis.
“It’s nice for those health care workers to feel appreciated by their communities,” she says. “It’s part of what gives them satisfaction for their jobs. It’s good for them and good for all of us.”
Jill hopes that prevails.
“That’s what we all need to continue to do,” she says. “A lot of people have been impacted by events this year. We all need to reach out and connect and look after each other a bit more.”
Original Article published by Edwina Mason on About Regional.