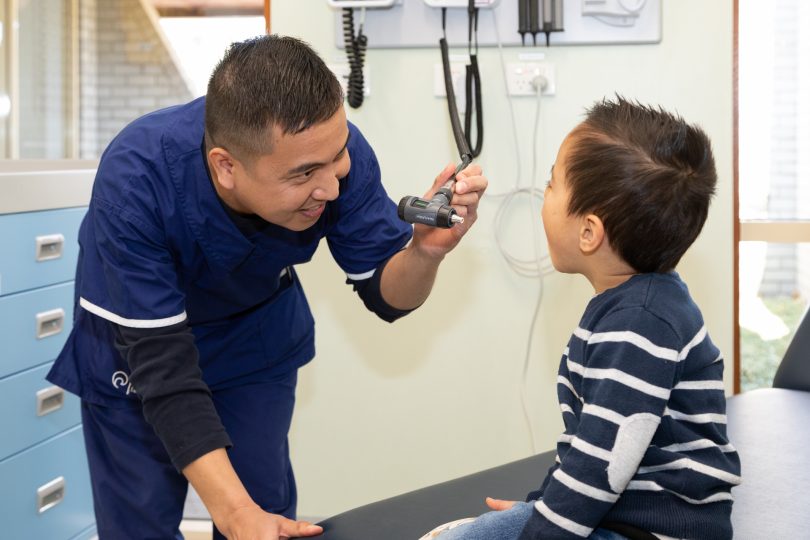
Advanced Practice Nurse Don Bernal and patient Nghia Tran at the Dickson Walk-in Centre. Five more centres are on the way. Photo: Region Media.
Doctors have welcomed government plans to widen the scope of new nurse-led Walk-in Centres but say the money would still be better spent on remedying the chronic problems in Canberra’s hospital emergency departments.
Ahead of the Budget on 9 February, the ACT Government announced yesterday (28 January) that it would add a further four centres to the five in the current network and the one promised for Coombs during the election campaign, all aimed at reducing the pressures in emergency departments (EDs).
Chief Minister Andrew Barr and Health Minister Rachel Stephen-Smith said the new centres, which would provide immediate care and appointment-based services, would ensure a good geographical spread of services close to where people live, especially in future growth areas.
It will spend $2 million on feasibility and site selection work for what it is now calling Walk-in Health Centres in South Tuggeranong, West Belconnen, the Inner South and North Gungahlin.
READ ALSO: Feds come through with $137 million to make Commonwealth Avenue Bridge safer
The feasibility study will investigate the potential to provide preventive health services, early intervention, and integrated care in the new centres.
And if the proposed new Walk-in Health Centre in Coombs is anything to go by they may be co-located with GP clinics. The Coombs centre will be co-located with the National Health Co-op GP clinic and open on 1 July.
The government will also spend $10.9 million in 2020-21 to include outpatient imaging services at the Weston Creek Walk-in Centre to reduce wait times in emergency and make it easier for the community to access common diagnostic imaging services.
ACT AMA president Dr Antonio Di Dio said doctors supported government attempts to make primary care as accessible and affordable as possible.
”They are trying to make them [walk-in centres] better value for taxpayers and more responsive to the needs of consumers,” he said.

Waiting times at the ACT’s EDs are the longest in the nation.
But Dr Di Dio said the government needed to define what it meant by integrated care and consult with local doctors, who were the experts in that field.
He said co-location would save the government money, but it needed to be open and transparent about the process and not upset established GP services.
The AMA has always maintained that the walk-in model represented poor value for money. Dr Di Dio said the government needed to put more money into key areas of the ACT’s hospitals to support EDs.
He said EDs did not need more staff, but hospitals needed more beds and staff in specialty areas such as mental health, which at times has overwhelmed the Canberra Hospital ED recently.
”You need more staff in different key areas so that when the ED doctors do their job, there’s a place to put [the patients].”
READ ALSO: Geocon revises Gungahlin project, but YMCA says it’s still too overbearing
The ED delays constantly reported in hospital data and the Productivity Commission’s Report on Government Services reflected the time it took between admittance and having a serviced bed available, Dr Dio said.
”A significant fraction of mental health patients might spend three days in the Canberra Hospital and the whole three days is in the ED because there is no bed upstairs to put them in,” he said.
”They opened an extra eight surge beds in Psychiatry a couple of weeks ago, but they were just pieces of furniture.”
Dr Di Dio said the budget needed to allocate more funds for the ACT’s hospitals, rather than on more Walk-in Centres.
”As a taxpayer and consumer, is this the most efficient way to spend our dollars? Could we spend it by employing a whole bunch of new people in the hospital that needs them?” he asked.
The Productivity Commission report on health services shows that the ACT’s ED waiting times are the longest in the country, and performance across several categories has deteriorated in recent years.




















